Introduction
- Importance of recognizing early signs and symptoms.
- The role of healthcare professionals in identifying abnormalities.
- How early detection can prevent complications.
Section 1: Definitions
- Sign: An objective, measurable indication of illness (e.g., fever, rash).
- Symptom: A subjective experience reported by the patient (e.g., pain, dizziness).
Section 2: General Signs and Symptoms
- Fever: Common in infections; understanding patterns (low-grade, high-grade, intermittent).
- Pain: Types (acute, chronic, localized, generalized).
- Fatigue: Causes (anemia, chronic conditions, stress).
- Nausea and Vomiting: Possible causes (gastrointestinal, neurological, infections).
- Cough: Types (dry, wet, chronic, acute) and related conditions (respiratory infections, allergies).
- Shortness of Breath (Dyspnea): Causes (asthma, pneumonia, cardiac issues).
- Swelling (Edema): Localized or generalized; common causes (injury, kidney issues, heart failure).
- Bleeding/Clotting Issues: Understanding the importance of platelet disorders or trauma.
Section 3: System-Specific Symptoms
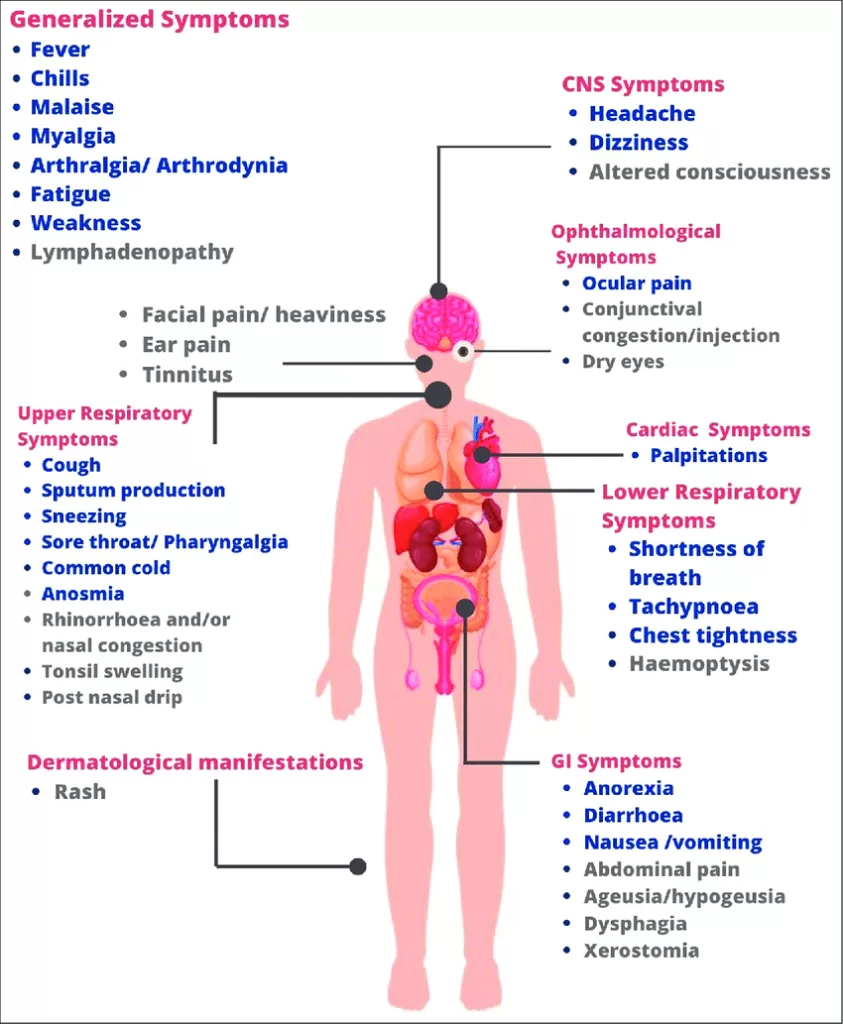
- Neurological:
- Headache.
- Dizziness/Vertigo.
- Numbness/Weakness.
- Seizures.
- Respiratory:
- Difficulty breathing (Dyspnea).
- Chest tightness.
- Hemoptysis (coughing blood).
- Cardiovascular:
- Palpitations ( Felling Slow or Fast Heartbeat )
- Chest pain (Angina).
- Swelling in legs.
- Gastrointestinal:
- Abdominal pain.
- Diarrhea/Constipation.
- Blood in stool (Melena or Hematochezia).
- Genitourinary:
- Painful urination (Dysuria).
- Change in urinary frequency.
- Blood in urine (Hematuria).
- Musculoskeletal:
- Joint pain or swelling.
- Muscle weakness or cramps.
- Skin:
- Rashes.
- Itching (Pruritus).
- Changes in skin color or texture.
Section 4: Assessment of Symptoms
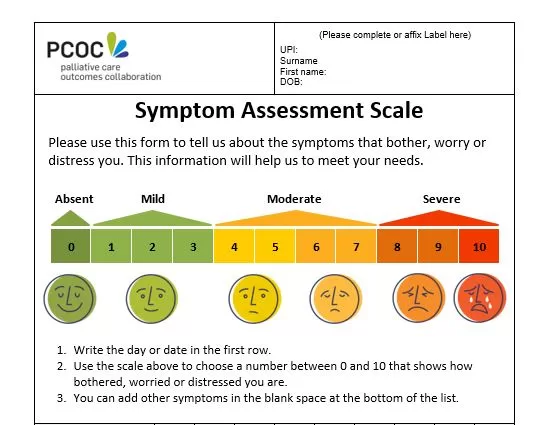
- Importance of history-taking:
- Duration, onset, and progression of symptoms.
- Associated factors (e.g., triggers, relievers).
- Observation and examination:
- Vital signs.
- Inspection, palpation, auscultation.
- Importance of patient communication:
- Active listening.
- Addressing patient concerns empathetically.
Section 5: Red Flags in Symptoms
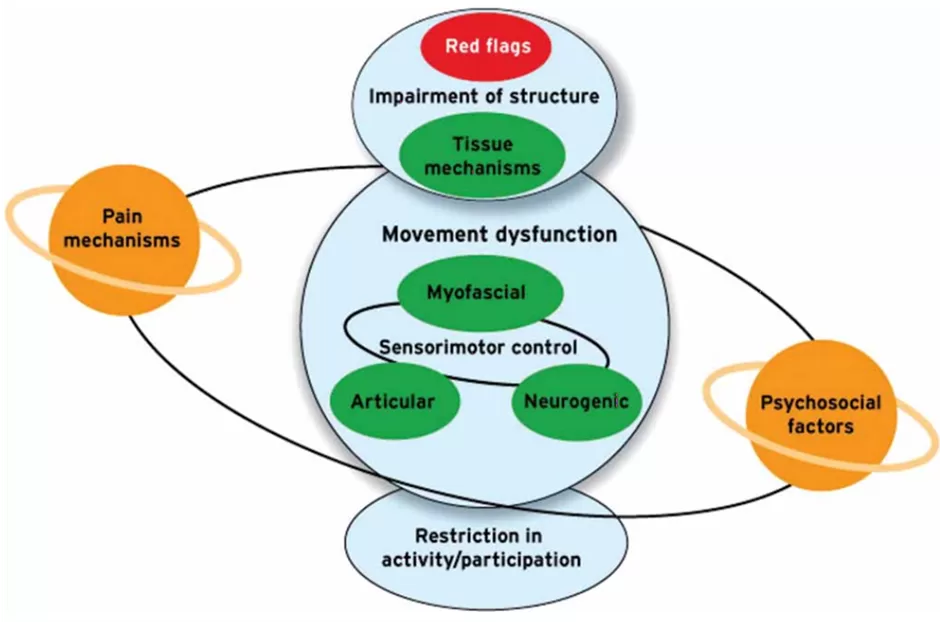
- Severe headache with sudden onset.
- Chest pain radiating to the arm or jaw.
- High fever with stiff neck or rash.
- Sudden loss of consciousness.
- Severe abdominal pain with vomiting.
Section 6: Documentation and Reporting
- Proper documentation of signs and symptoms.
- Reporting to seniors or doctors for timely intervention.
Section 1: General Symptoms
General symptoms are often non-specific but critical indicators of illness. These include:
- Fever:
- Body temperature exceeding normal ranges (above 37.5°C/99.5°F).
- Common in infections, autoimmune disorders, and malignancies.
- Pain:
- Types: Acute, chronic, localized, generalized.
- Causes: Inflammation, injury, infection.
- Fatigue:
- Persistent tiredness despite rest.
- Linked to anemia, thyroid dysfunction, or chronic diseases.
- Weight Loss/Gain:
- Unintentional changes in weight due to metabolic disorders, cancers, or hormonal imbalances.
- Appetite Changes:
- Loss of appetite (anorexia) or increased hunger (polyphagia).
- Associated with conditions like diabetes, infections, or psychological issues.
- Nausea and Vomiting:
- Common in gastrointestinal, neurological, or metabolic conditions.
- Dizziness/Vertigo:
- Linked to vestibular disorders, dehydration, or low blood pressure.
- Sweating (Diaphoresis):
- Night sweats in infections or excessive sweating in thyroid disorders.
Section 2: Altered Vital Signs
Vital signs are key indicators of a patient’s physiological status. Changes can signal acute or chronic conditions.
- Temperature:
- Hyperthermia (Fever): Infection, inflammation, heatstroke.
- Hypothermia: Exposure to cold, hypothyroidism, or shock.
- Pulse/Heart Rate:
- Tachycardia (Fast heart rate): Dehydration, fever, stress.
- Bradycardia (Slow heart rate): Hypothyroidism, heart block.
- Respiratory Rate:
- Tachypnea (Increased rate): Anxiety, lung infection, acidosis.
- Bradypnea (Decreased rate): Drug overdose, brain injury.
- Blood Pressure:
- Hypertension: Stress, kidney disease, cardiovascular disorders.
- Hypotension: Shock, dehydration, or blood loss.
- Oxygen Saturation (SpO₂):
- Decreased levels indicate hypoxemia, common in respiratory or cardiac conditions.
Section 3: Skin Changes
The skin often reflects systemic illnesses. Key signs include:
- Color Changes:
- Pallor: Anemia or poor circulation.
- Cyanosis: Low oxygen levels in blood (bluish discoloration).
- Jaundice: Yellowing due to liver disease or hemolysis.
- Redness (Erythema): Inflammation, fever, or infections.
- Texture Changes:
- Dryness: Dehydration, hypothyroidism.
- Scaling: Psoriasis, fungal infections.
- Thickening: Chronic dermatitis or lymphedema.
- Rashes:
- Macules, papules, pustules, vesicles (linked to allergies, infections).
- Lesions:
- Wounds, ulcers, or abnormal growths.
- Bruising (Ecchymosis):
- Indicates trauma, clotting disorders, or abuse.
- Itching (Pruritus):
- Can occur in liver diseases, allergies, or kidney failure.
- Swelling:
- Localized: Infections, bites.
- Generalized: Edema in kidney or heart diseases.